COVID-19 outbreak is a pandemic. The number of severe acute respiratory syndrome coronavirus2 (SARS-CoV-2) infection is increasing rapidly and results in high rates of hospitalization and intensive care unit (ICU) admission. Coagulopathy is an important complication of COVID-19, which increased the mortality. The national medical team of PUMCH published a correspondence article “Coagulopathy and Antiphospholipid Antibodies in Patients with COVID-19” online in “The New England Journal of Medicine” on April 8th, 2020. Professor. Shuyang Zhang and Yongzhe Li are the correspondence authors. This is the first report of antiphospholipid antibodies (aPLs) observed in critically ill patients with COVID-19, and reveals that the abnormities of autoimmune system are related with coagulopathy and thrombosis formation closely.
The national medical team of PUMCH came to Wuhan since January 26th,2020,and managed the intensive care unit of Sino–French New City Branch of Tongji Hospital. The ward was set up on an emergency basis to accept the most critically ill patients during the outbreak of COVID-19. PUMCH multidisciplinary team found that the significantly hypercoagulable status was widely existed in these critical patients, and the clinical manifestations of occlusion and microthrombosis formation were observed, including cyanosis and acro-ischemia. Based on the support of MDT consult from PUMCH, the frontline work team formulated the standardized approach to thrombosis evaluation and anticoagulation therapy.

President Yupei Zhao officiated the MDT meeting
At the same time, the scientific research team began to explore the etiology of hypercoagulable status. As early as 17 years ago, Yongzhe Li, the professor of clinic laboratory department, found the emerge of aPLs in patients with SARS infection during the SARS outbreak in 2003. Considered the similarity of SARS-Cov-2 and SARS, the similar autoimmune reactions may occur during SARS-Cov-2 infection. An integrated autoimmune storm research program was started as soon as possible. According to the clinical signs and laboratory abnormalities, Yan Zhang, Meng Xiao and other young doctors joined the program, reviewed the clinical data and carried out a series of autoimmune antibodies and cytokine tests to interpret the relationship between autoimmune storm and coagulation system activation.
The preliminary results demonstrated that nearly 40% critical patients admitted to ICU had aPLs without other autoantibodies, and several patients developed severe thrombotic events, including cerebral infarction, jugular thrombosis and so on. After a profound discussion by the experts of hematology, rheumatology, neurology and cardiology, the consensus was achieved: the emerge of aPLs was induced by virus infection, the lower titer antibody was likely transient without definite clinical significance. Meanwhile the high titer antibodies with multiple isotypes are probably related with thrombotic events and secondary antiphospholipid syndrome should be considered in these patients.
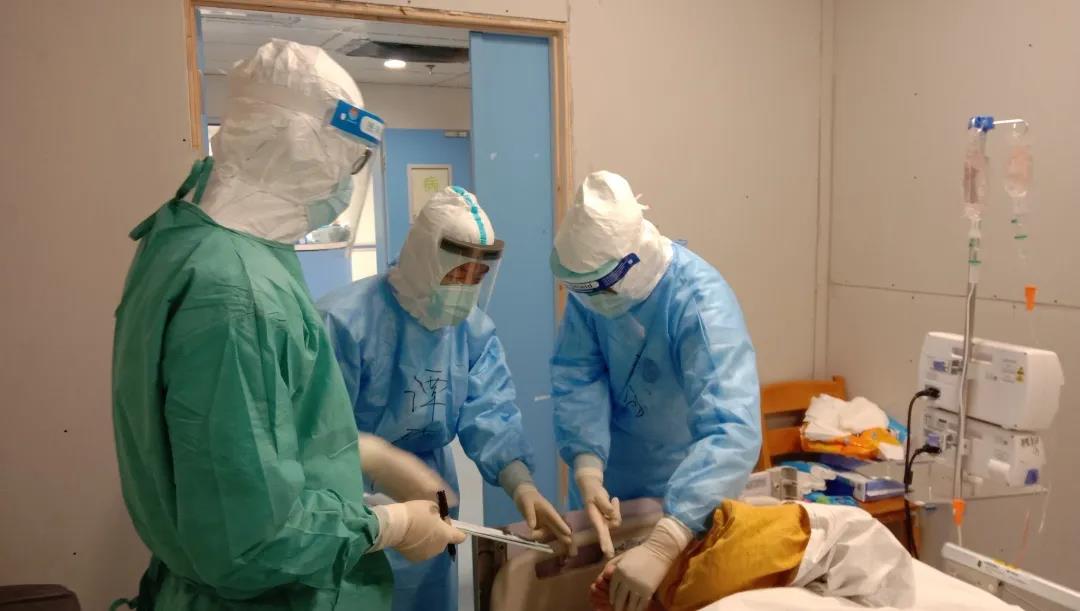
The national medical team of PUMCH exploring the standard anticoagulation treatment
The PUMCH national medical team summarized the clinical and laboratory characters of 3 patients, and published the relationship between aPLs and coagulopathy for the first time in the world. The result demonstrated that multiple mechanisms are implicated in the development to hypercoagulable status in critically ill patients with COVID-19, and the appearance of aPLs exacerbates the coagulopathy. Catastrophic APS may be developed in individual patients. Anticoagulation therapy is essential for these patients, and anti-platelet therapy should be added to reduce the risk of arterial thrombosis. On the other hand, the appearance of aPLs implies the turbulence of autoimmune system after SARS-Cov-2 infection, and these patients should be followed up for a long time to evaluated the risk of autoimmune disorders.




PUMCH MDT of experts working in Wuhan national medical team as well as those in Beijing home base discussing disseminated intravascular coagulation (DIC) symptoms of critically ill COVID-19 patients.
https://www.nejm.org/doi/full/10.1056/NEJMc2007575?query=featured_home
Writer: Yan Zhang, Meng Xiao
Editor: Tan-ping Fu
Photo: Peng-fei Wang, PUMCH national medical team members
