On March 26, 2026, the team led by Chen Youxin, Chief Physician of the Department of Ophthalmology at PUMCH, in collaboration with Professor Sheng Bin's team from Shanghai Jiao Tong University, published their latest research findings in The Lancet Digital Health (a tier 1 journal ranked among the top 5% by the Chinese Academy of Sciences, IF: 24.1). The study presents the development and validation of a deep learning model called the KongMing Model (a structural-attention guided therapeutic response predicting model), aiming to predict visual and anatomical prognoses in patients with neovascular age-related macular degeneration (nAMD) undergoing anti-vascular endothelial growth factor (anti-VEGF) therapy, offering a powerful decision-support tool for nAMD management.

This study was led by the Department of Ophthalmology at PUMCH and conducted in collaboration with 18 tertiary hospitals across 12 provinces nationwide. The core innovation lies in a lesion-aware, transformer-based multitask model architecture. The model was composed of three tightly coupled modules: a best-corrected visual acuity (BCVA) change classification (improvement, stability, or deterioration) module, a BCVA value regression module and a post-treatment optical coherence tomography (OCT) image generation module.The prognosis assessments cover three clinically critical time points at post-single-injection, post-three-loading-injections, and 1-year post-3+PRN treatment, providing comprehensive short-, medium-, and long-term prognostic assessment.

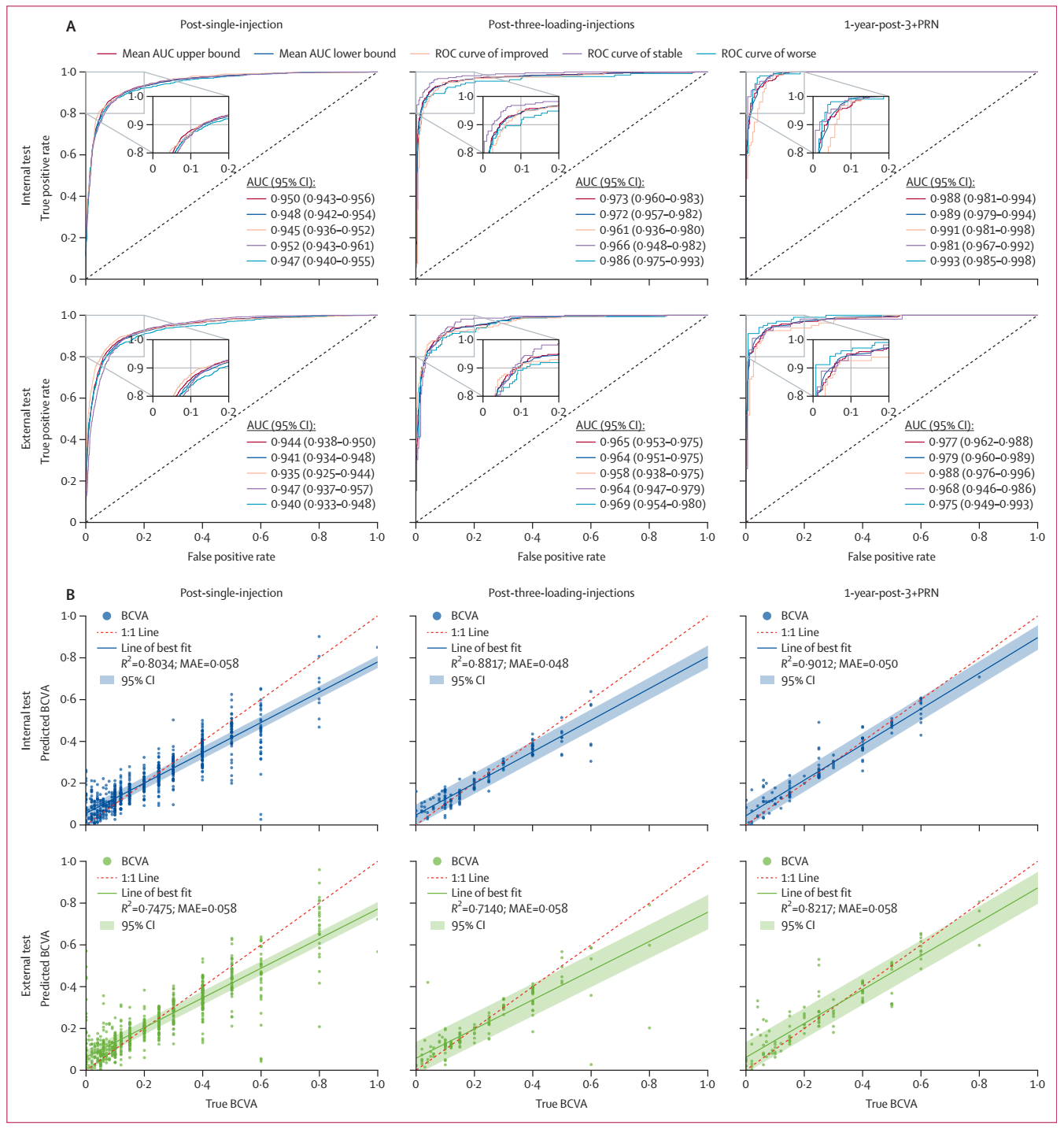
The model demonstrated outstanding overall performance. In predicting BCVA changes, it significantly outperformed clinicians in accuracy. BCVA value predictions showed low mean absolute error (MAE), and the model generated images with close similarity to actual outcomes. Compared with established baseline models, the KongMing Model achieved consistent improvements across all evaluation metrics. The model is also capable of identifying key imaging features associated with prognosis, with findings that align closely with conclusions from prior research.
Compared with baseline models, the KongMing Model demonstrated significant advantages across all evaluation metrics. The model was able to precisely locate imaging biomarkers associated with prognosis. Specifically, conventional choroidal neovascularisation, old scars, and intraretinal fluid were all associated with poor prognoses, whereas subretinal fluid correlated with favourable outcomes. The model also identified features such as polyp-like fibrovascular pigment epithelial detachment and focal choroidal excavation — OCT biomarkers consistent with those reported in the existing literature.
The researchers highlight that by accurately predicting individualized treatment outcomes, the KongMing Model can support shared decision-making between clinicians and patients, improve treatment adherence, and help avoid unnecessary interventions. For patients showing an inadequate early response, treatment strategies can be adjusted promptly; for those predicted to respond well, the model can reinforce their confidence in continuing therapy. This holds great significance for reducing the medical burden on patients and optimizing the allocation of healthcare resources.
The co-first authors of this paper are Zhao Xinyu, Attending Physician in the Department of Ophthalmology at PUMCH; Wen Yang, Distinguished Associate Researcher at the College of Electronics and Information Engineering, Shenzhen University; and Yang Zuyi, a Class of 2020 student in the eight-year program of clinical medicine at Peking Union Medical College. The co-corresponding authors are Chen Youxin and Sheng Bin.
